

A safety assessment code matrix will help your organization rank hazards and vulnerabilities that could result in patient harm, as well as consistently and transparently decide which event or risks to study and mitigate first. Building the matrix should be a team effort and endorsed by the facility’s leadership.
Here's what the safety assessment code matrix looks like. This originated with the National Center for Patient Safety of the US Department of Veterans Affairs. Your matrix may need to be adapted to your facility's setting, regulatory environment, and/or applicable accreditation standards.
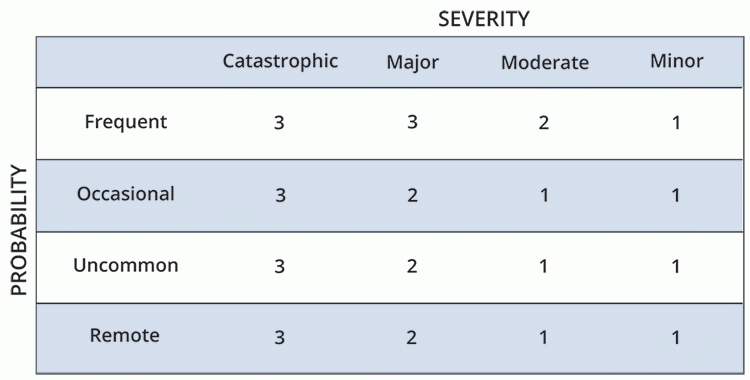
Start by determining the severity of the event or a close call (sometimes referred to as a 'near miss'). Was it catastrophic, major, moderate, or minor? Key factors to consider include: extent of injury, length of stay, level of care required for remedy, and known or estimated physical plant costs.
Some helpful criteria you can use:
As with the severity categories, the probability categories apply to actual adverse events and close calls.
To assign a probability rating, it is ideal to know how often the event for close call occurs at your facility. Sometimes the data will be easily available because they are routinely tracked (e.g., falls with injury, adverse drug events, etc.). Other times, you will need to ask for an informal opinion from other staff or default to your own best educated guess.
Use these probability terms and criteria:
Frequent – Likely to occur immediately or within a short period (may happen several times in 1 year).
Occasional – Probably will occur (may happen several times in 1 to 2 years).
Uncommon – Possible to occur (may happen sometime in 2 to 5 years).
Remote – Unlikely to occur (may happen sometime in 5 to 30 years).
Look at where the severity column and risk row intersect. That is the score of the event or close call.
Click here for an example of how to use the matrix.
Source: Excerpted and adapted from Bagain JP, Lee CZ, Cole, JF, “A Method for Prioritizing Safety Related Actions,” in Strategies for Leadership: A Toolkit for Improving Patient Safety, developed by the Department of Veterans Affairs National Center for Patient Safety, sponsored by the American Hospital Association.